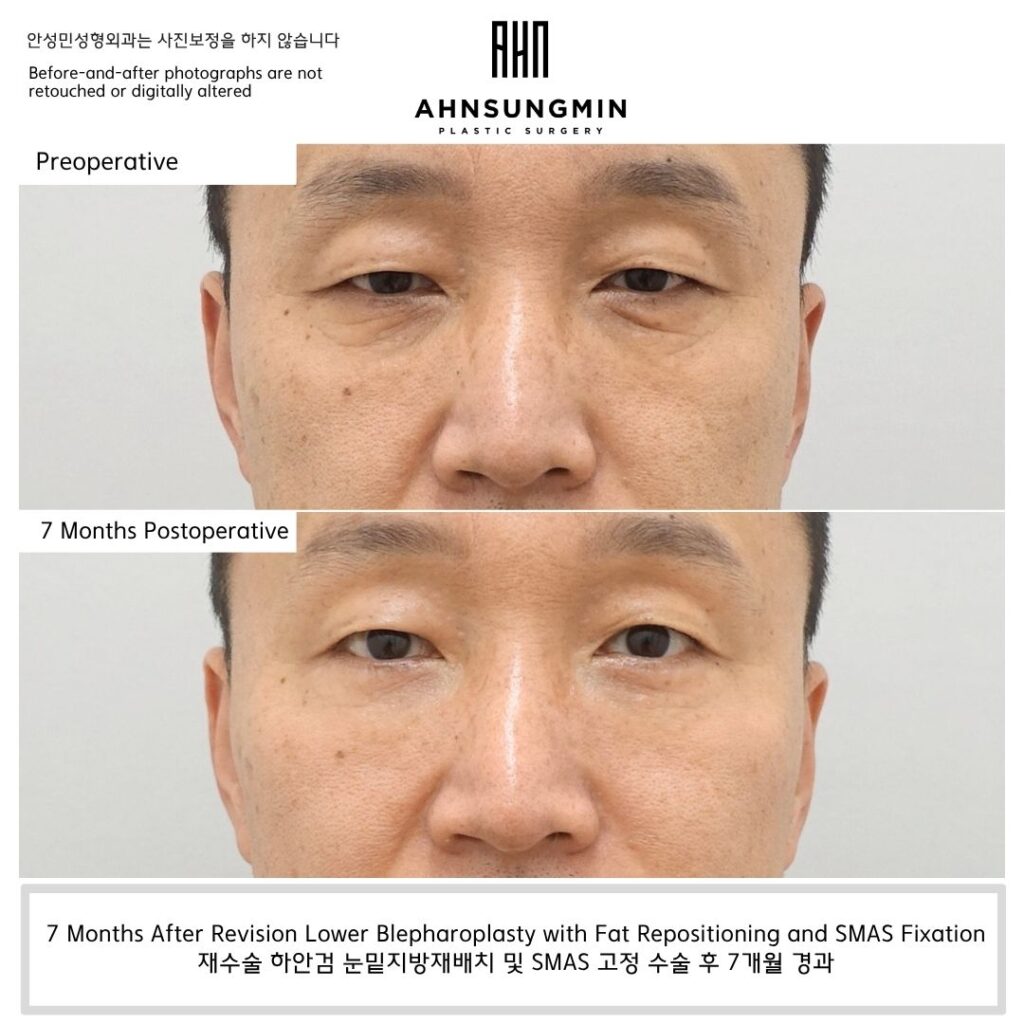
Before and After
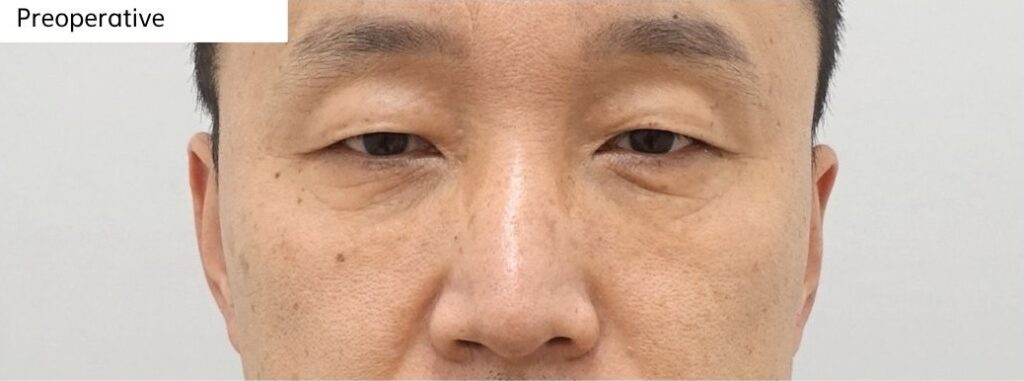
[Before Photo]
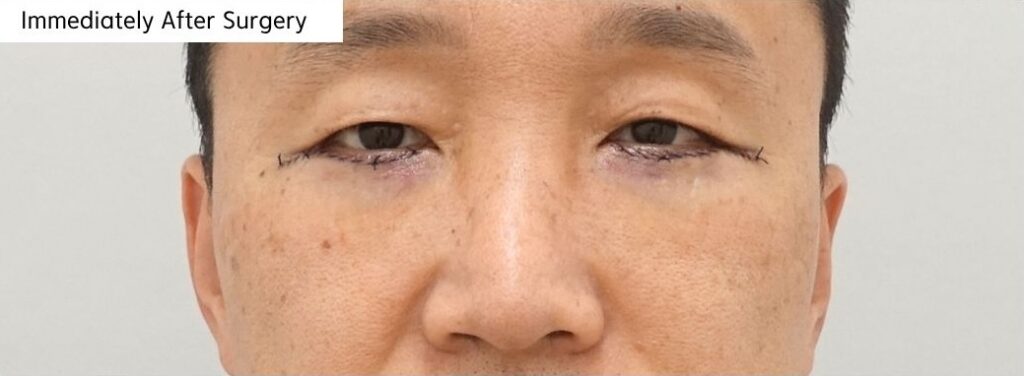
[Immediately After Surgery Photo]
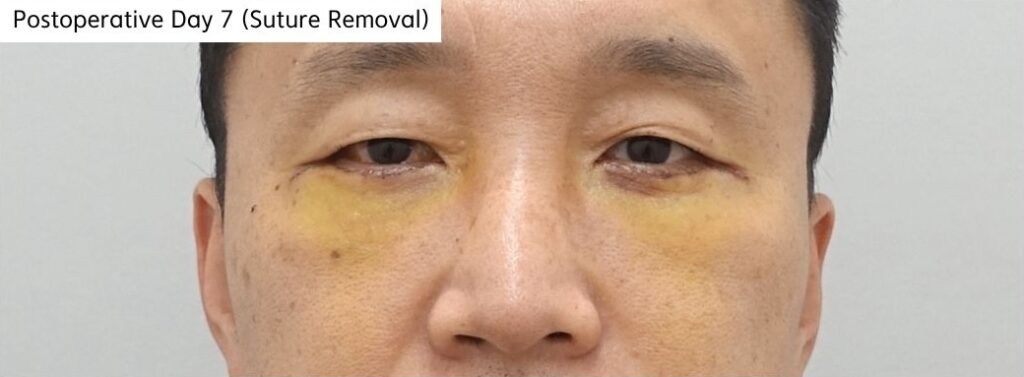
[Postoperative Day 7 Photo]
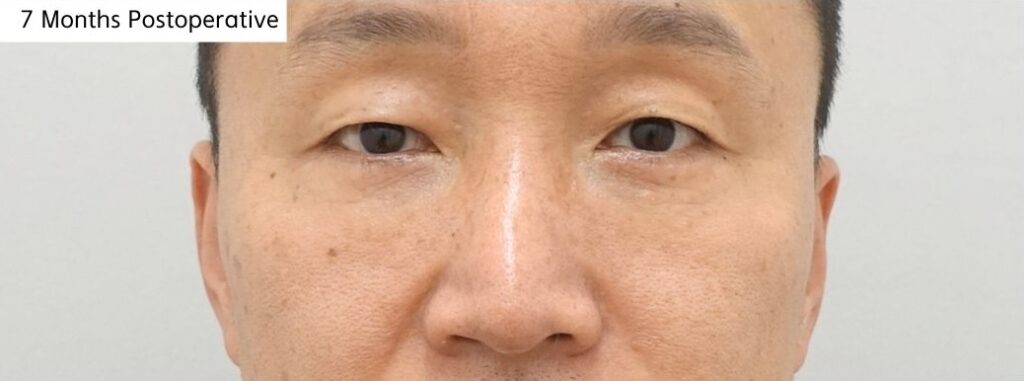
[3 Months Postoperative Photo]
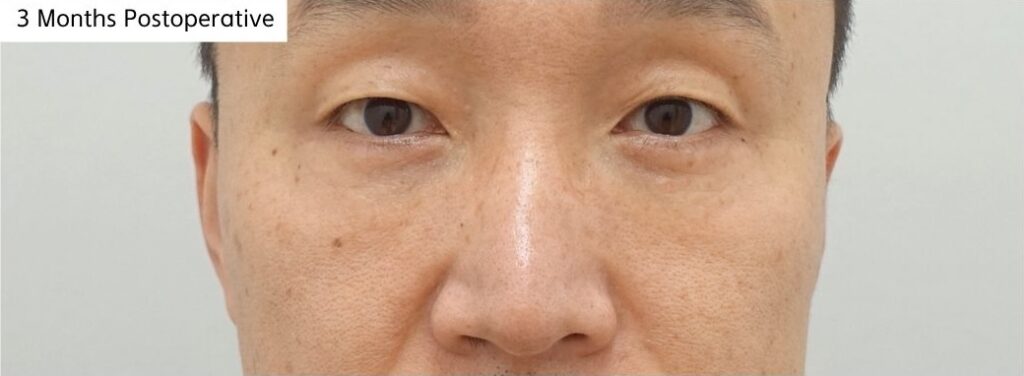
[7 Months Postoperative Photo]
Why This Patient Required Revision Lower Blepharoplasty
This patient previously underwent lower eyelid surgery but continued to experience persistent under-eye bulging, contour irregularity, and incomplete volume transition beneath the eyes.
In many revision lower blepharoplasty cases, the original issue is not simply “remaining fat.”
More often, the problem involves imbalance between protruding fat, weakened lower eyelid support, volume loss, and structural instability that develops after aggressive tissue removal or incomplete repositioning.
Revision surgery around the lower eyelid is significantly more complex than primary surgery because scar tissue, adhesion, altered anatomy, and weakened support structures must all be carefully evaluated before any correction is attempted.
Rather than pursuing excessive tightening or additional fat removal, this revision procedure focused on restoring lower eyelid support and rebuilding smoother volume continuity beneath the eyes.
Why Aggressive Fat Removal Was Avoided
One of the most common long-term problems after lower eyelid surgery is excessive hollowing caused by over-resection of orbital fat.
When too much fat is removed, the under-eye area may initially appear flatter but gradually becomes more hollow, sharper, and structurally aged over time.
In revision surgery, this problem often becomes even more apparent because tissue elasticity and support are already compromised from prior surgery.
For this reason, fat preservation and structural fat repositioning were prioritized instead of aggressive excision.
The goal was not to create an artificially tight lower eyelid, but to restore smoother contour transition while maintaining long-term stability and natural facial balance.
Structural Support Was More Important Than Tightness
Revision lower blepharoplasty requires more than cosmetic adjustment alone.
In this case, SMAS fixation and structural reinforcement were performed together with fat repositioning to stabilize the lower eyelid and reduce downward tension during healing.
Many patients believe tighter skin automatically creates better results.
However, excessive tension may actually increase the risk of lower eyelid stiffness, prolonged swelling, unnatural contour, or lower eyelid malposition over time.
Long-term stability often depends more on structural support and balanced healing than aggressive tightening itself.
Recovery Process After Revision Lower Blepharoplasty
Immediately after surgery, temporary swelling and bruising were visible around the lower eyelids.
At postoperative day 7, bruising remained present but early contour stabilization had already begun to appear.
By 3 months, most visible swelling had improved significantly, and the under-eye contour appeared softer and more balanced.
At 7 months, the lower eyelid contour demonstrated more stable volume transition and improved structural harmony without excessive hollowness or tightness.
Recovery after revision lower blepharoplasty is often slower than primary surgery because tissue healing occurs within previously operated anatomy and scar tissue.
Patients considering revision surgery should understand that lower eyelid stabilization continues gradually over many months beneath the surface.
To better understand how recovery evolves over time after surgery, review our
Lower Blepharoplasty Recovery Timeline in Korea.
Surgical Approach
Revision lower blepharoplasty was performed with a focus on structural correction, volume preservation, lower eyelid support, and long-term stability rather than excessive fat removal or aggressive skin tightening.
Because revision lower eyelid surgery involves scar tissue and altered anatomy from previous procedures, surgical restraint and tissue preservation are often more important than aggressive correction.
Lower Eyelid Revision Surgery FAQ
Why do patients require revision lower blepharoplasty?
Revision surgery may become necessary when persistent bulging, hollowing, asymmetry, scar adhesion, contour irregularity, or lower eyelid weakness remain after prior surgery.
Why was fat repositioned instead of removed again?
Additional fat removal in revision surgery may worsen hollowing and structural instability. Fat repositioning often creates a smoother and more natural lower eyelid contour while preserving support.
Is revision lower blepharoplasty more difficult than primary surgery?
Yes. Scar tissue, altered anatomy, tissue stiffness, and weakened support structures make revision lower eyelid surgery significantly more complex than first-time surgery.
Does swelling last longer after revision surgery?
In many cases, yes. Healing after revision surgery often progresses more slowly because tissues have already undergone previous surgical changes.
When do revision lower eyelid results become stable?
Visible recovery improves gradually during the first several weeks, but deeper tissue stabilization and scar maturation may continue for several months after revision surgery.
Request a Revision Lower Eyelid Surgery Evaluation
Revision lower eyelid surgery requires careful structural analysis rather than aggressive correction alone.
Previously operated tissues often involve scar adhesion, altered anatomy, weakened support structures, and long-term volume imbalance.
If you are considering revision lower blepharoplasty in Korea, you may request a personalized evaluation based on your previous surgical history, current lower eyelid condition, tissue stability, and long-term recovery potential.
